Chief Medical Officers, CEOs, and other key decision-makers in modern primary care want to support Primary Care Providers (PCPs) so they can meet the physical and mental health needs of their patients. But limited time, resources, and mental health expertise lead 79% of PCPs to burnout, resulting in poorer quality care for their patients and an industry on the brink of failure.
To ensure our collective well-being, we invite healthcare leaders to partner with evolvedMD and leverage its enhanced Psychiatric Collaborative Care Model (CoCM) to better support their PCPs and drive improved patient outcomes for thriving communities nationwide.
What is evolvedMD’s enhanced Psychiatric CoCM?
We believe patients are best served when primary care and behavioral health work together. Our enhanced approach to Psychiatric CoCM achieves this by placing our Behavioral Health Managers (licensed therapists and social workers) on-site and in-person (or virtual if needed) at each of the practices we serve, fully embedding them within a collaborative team led by a Primary Care Provider.
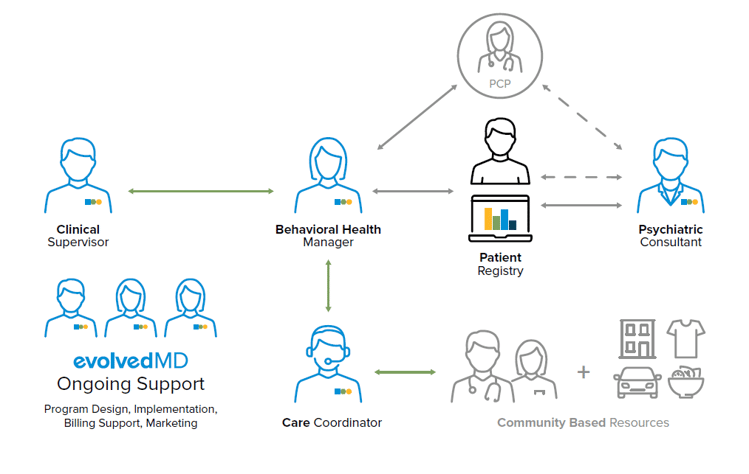
Key Figures Explained
- Behavioral Health Manager – Sees patients onsite and in-person as a member of the primary care practice’s team.
- Psychiatric Consultant – Provides additional clinical support including medication management and elevated consults.
- Clinical Supervisor – Provides clinical supervision and supports practice manager.
- Care Coordinator – Supports BHM’s administrative needs and connects patients to additional community resources.
- evolvedMD Ongoing Support – Monitors, enhances, and continuously improves program.
- Patient Registry – Central hub for on-demand access to patient’s most current clinical information, including diagnosis, medications, etc.
Not only does the enhanced Psychiatric CoCM better serve patients, but it also better serves providers and primary care groups compared to traditional settings.
How does evolvedMD’s enhanced Psychiatric CoCM model benefit providers and primary care groups?

- It empowers providers to drive improved patient outcomes
Providers are responsible for treating physical health symptoms and now more than ever, mental health symptoms given the harrowing state of mental health. However, limited time, training, and support from qualified mental health professionals prevent them from effectively treating the whole patient. Knowing that mental health impacts physical health and is integral to living a balanced life, the enhanced Psychiatric CoCM model complete with trained mental health professionals onsite, enables providers and their collaborative teams to effectively treat the whole patient, improving patient outcomes and satisfaction with care.
- It streamlines communication and collaboration
A lack of communication and close collaboration can cause worse clinical outcomes and decreased patient satisfaction. The enhanced Psychiatric CoCM promotes continuity of care and clarity among the provider’s collaborative team to close communication gaps and consistently deliver a high-quality experience.
- It provides upfront, ongoing support from behavioral health integration experts
While Primary Care Providers can treat common mental health issues, they have limited time and expertise, which often makes them refer patients out for mental health care. Through the enhanced Psychiatric CoCM, the provider’s collaborative care team can lend behavioral health expertise and support onsite so they aren’t responsible for coordinating all levels of care. Additionally, instead of referring patients out for mental health treatment, CoCM will keep patients where they’re most comfortable: at their preferred primary care practice where they visit their trusted provider.
- It promotes shared learning between providers and mental health professionals
The inability to share knowledge leads to worse-quality whole-person care. Shared learning between physical and mental health professionals will enhance the provider’s ability to solve problems, make decisions, and develop cohesive care plans for their patients. evolvedMD’s team is available for ongoing mental health education with a clinically-validated curriculum rooted in behavioral health for primary care.
- It improves provider well-being
Increased patient demand, long hours, and limited time and space to practice self-care leads to burnout, resulting in poorer-quality care. With a collaborative care team to manage workloads, Primary Care Providers will have more time and space to practice self-care and prevent burnout (evolvedMD's Dr. Ruth Nutting, Director of Clinical Programs, recently published research about how practicing mindfulness can improve physicians' health and well-being). Additionally, evolvedMD’s Behavioral Health Managers are also available to provide quick support and wellness information for providers. By partnering with evolvedMD and embedding our team of behavioral health experts into your provider’s collaborative care team, your practice can offer a comprehensive solution that not only benefits patients but your providers, too.
Partner with evolvedMD today to bring our
enhanced Psychiatric CoCM to your practice.